Welcome to LSB Courses Blog
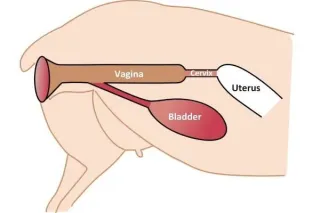
Prolapse in sheep - how to empty the bladder
Dealing with a prolapsed ewe? The first critical step before the vet arrives is to empty her bladder. Learn why this is essential, how to do it safely, and how it can prevent complications like toxic ... ...more
Practical skills
March 01, 2025•2 min read

Natural worm control in livestock
Worm burdens in livestock can significantly impact animal health and productivity. Traditionally, chemical drenches have been the go-to solution, but overuse has led to widespread drench resistance. ...more
Practical skills
November 04, 2024•5 min read

Protecting Your Backyard Poultry from HPAI H5N1
You have probably seen recent headlines about a worrying new bird flu strain. The catchily named HPAI H5N1 has been making headlines globally due to its high mortality rate and its ability to spread. ...more
Did you know?
July 26, 2024•3 min read
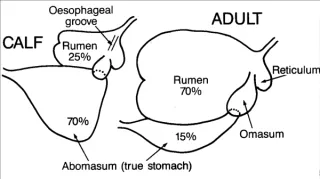
Why tube feeding should be your last option
If a newborn livestock animal is too weak to suckle then often the only option appears to be to tube feed colostrum but there are very good reasons why this should be your last option - not a ‘go-to’. ...more
Background basics
June 18, 2024•5 min read

Basic Needs for Sheep
The rural dream has become a reality and you have decided to buy some sheep. So, what are the basic needs for our ovine friends? ...more
Background basics ,Practical skills
May 28, 2024•5 min read

Help my chook is broody!
How to care for your broody hen, and how to curb broody behaviours in the future if you don't want chicks. ...more
Background basics
May 13, 2024•5 min read
© 2024 LSB Ltd. All Rights Reserved.

